A recent study by researchers at the Max Planck Institute for Infection Biology, the Pasteur Institute and the International Center for Research in Infection (CIRI) indicates that the spread of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) is affected by influenza. Infection with the virus during the initial period of the 2019 Coronavirus (COVID-19) epidemic in Europe. The study is currently available on medRxiv * Server preprint.
Since its appearance in December 2019 in China, the highly prevalent SARS-CoV-2 virus has infected more than 27.99 million people worldwide and killed 906,122 people. Due to the lack of adequate curative interventions or vaccinations, many preventive measures have been taken to address the epidemic, such as nationwide lockdowns in more than 100 countries.
Regarding potential risk factors, several studies have shown that the elderly, male individuals, and people with comorbidities (cardiovascular and / or lung disease, diabetes, kidney disease, and cancer) are more likely to develop a severe form of COVID-19, which is associated with a higher mortality rate. .
![Potential drivers of SARS-CoV-2 transmission in Belgium, Italy, Norway and Spain. A: A timeline for the Agility Index, which is a nationwide aggregate measure of the number and severity of non-pharmaceutical control measures implemented by governments. The dashed vertical line indicates the start of the nationwide lockdown [16]. B: Influenza incidence timeline, computed as the product of the incidence of influenza-like illness and breakdown of positive samples for any influenza virus (see also Figure S1 for a timeline of the last two variables). Vertical dashed lines define the period of interference between SARS-CoV-2 and influenza, defined as the period between the assumed start date of community transmission of SARS-CoV-2 and 6 weeks after the peak of an influenza pandemic [46]. In each country, the time series presented were incorporated as covariates, which modulated the SARS-CoV-2 transmission rate in our model (see Methods). In B, the y-axis values differ for each plate. Potential drivers of SARS-CoV-2 transmission in Belgium, Italy, Norway and Spain. A: A timeline for the Agility Index, which is a nationwide aggregate measure of the number and severity of non-pharmaceutical control measures implemented by governments. The dashed vertical line indicates the start of the nationwide lockdown [16]. B: Influenza incidence timeline, computed as the product of the incidence of influenza-like illness and breakdown of positive samples for any influenza virus (see also Figure S1 for a timeline of the last two variables). Vertical dashed lines define the period of interference between SARS-CoV-2 and influenza, defined as the period between the assumed start date of community transmission of SARS-CoV-2 and 6 weeks after the peak of an influenza pandemic [46]. In each country, the time series presented were incorporated as covariates, which modulated the SARS-CoV-2 transmission rate in our model (see Methods). In B, the y-axis values differ for each plate.](https://news.google.com/image.axd?picture=2020%2f9%2f%40_2020.09.07.20189779v1.jpg)
Potential drivers of SARS-CoV-2 transmission in Belgium, Italy, Norway and Spain. A: A timeline for the Agility Index, which is a nationwide aggregate measure of the number and severity of non-pharmaceutical control measures implemented by governments. The dashed vertical line indicates the start of the nationwide lockdown. B: A timeline of the occurrence of influenza, computed as the product of the occurrence of influenza-like illnesses and breakdown of positive samples for any influenza virus. The vertical dashed lines define the period of interference between SARS-CoV-2 and influenza, which was defined as the period between the assumed start date of transmission of the SARS-CoV-2 community and 6 weeks after the peak of the influenza pandemic. In each country, the time series presented as covariates were incorporated, which modulate the SARS-CoV-2 transmission rate in the model. In B, the y-axis values differ for each plate.
The hypothesis of the study
With regard to seasonal viral infection in the human respiratory system, evidence indicates that the interaction between pathogens circulating during a pandemic or epidemic can be beneficial or unfavorable in terms of virus spread or disease severity. For example, infection caused by influenza virus has been shown to prevent secondary infection caused by respiratory syncytial virus in rodents. In contrast, there is evidence to suggest that respiratory influenza infection can increase expression of angiotensin converting enzyme 2 (ACE2), a receptor in the respiratory epithelium that interacts with the SARS-CoV-2 protein and facilitates virus entry. In human cells.
Given the important past experience about the impact of existing pathogens on the spread to the pandemic, the scientists of the current study hypothesized that the common influenza virus may have influenced the spread of SARS-CoV-2 in Europe during the initial phase of the Covid-19 pandemic.
study design
Scientists have developed a population-based randomized model for SARS-CoV-2 transmission and COVID-19 related deaths. Assuming death occurred in 1% of all infections, the scientists combined a representative distribution of virus generation time, duration between symptom onset and death into their model. It also incorporated the rigor index, which is a measure of the number of control measures (lockdowns, workplace / school closures, travel restrictions, etc.) that governments have taken during the pandemic and their strictness. They evaluated the effect of the severity index on virus spread. The effect of influenza infection on the prevalence of SARS-CoV-2 was assessed by incorporating a time series analysis of influenza incidence into the model. Information on influenza cases in four European countries, including Belgium, Italy, Norway and Spain, was obtained from the World Health Organization.
![Potential drivers of SARS-CoV-2 transmission in Belgium, Italy, Norway and Spain. A: A timeline for the Agility Index, which is a nationwide aggregate measure of the number and severity of non-pharmaceutical control measures implemented by governments. The dashed vertical line indicates the start of the nationwide lockdown [16]. B: Influenza incidence timeline, computed as the product of the incidence of influenza-like illness and breakdown of positive samples for any influenza virus (see also Figure S1 for a timeline of the last two variables). Vertical dashed lines define the period of interference between SARS-CoV-2 and influenza, defined as the period between the assumed start date of community transmission of SARS-CoV-2 and 6 weeks after the peak of an influenza pandemic [46]. In each country, the time series presented were incorporated as covariates, which modulated the SARS-CoV-2 transmission rate in our model (see Methods). In B, the y-axis values differ for each plate. Potential drivers of SARS-CoV-2 transmission in Belgium, Italy, Norway and Spain. A: A timeline for the Agility Index, which is a nationwide aggregate measure of the number and severity of non-pharmaceutical control measures implemented by governments. The dashed vertical line indicates the start of the nationwide lockdown [16]. B: Influenza incidence timeline, computed as the product of the incidence of influenza-like illness and breakdown of positive samples for any influenza virus (see also Figure S1 for a timeline of the last two variables). Vertical dashed lines define the period of interference between SARS-CoV-2 and influenza, defined as the period between the assumed start date of community transmission of SARS-CoV-2 and 6 weeks after the peak of an influenza pandemic [46]. In each country, the time series presented were incorporated as covariates, which modulated the SARS-CoV-2 transmission rate in our model (see Methods). In B, the y-axis values differ for each plate.](https://news.google.com/image.axd?picture=2020%2f9%2f%402020.09.07.20189779v1.jpg)
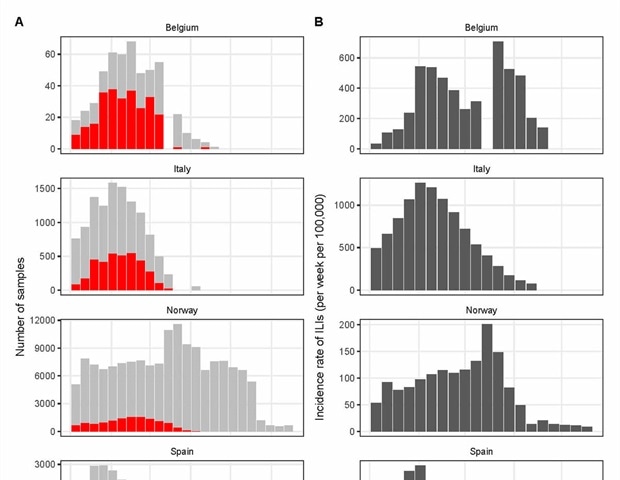
Data on suspected influenza syndromic (A) and influenza virus (B) data for Belgium, Italy, Norway and Spain. In A, the red bars represent the number of positive samples for any influenza virus and the gray bars that are negative.
Important notes
Scientists have consistently observed that there is a 2–2.5-fold increase in SARS-CoV-2 transmission during the period that the influenza virus and SARS-CoV-2 have been present together. Regarding control measures, they found that strict implementation of control measures was associated with reduced transmission of the virus.
Based on the descriptive statistical analysis of the model data, the scientists believe that their model effectively predicted the morbidity and mortality associated with SARS-CoV-2 over the study period.
Predictions given by the study model
Based on the model data, scientists predicted that people who had recently had an influenza infection were more likely to develop SARS infection. This prediction was justified by previous study observations showing higher transmissibility or susceptibility in persons infected with influenza virus and SARS-CoV-2.
Studies investigating the frequency of co-diagnosis of influenza polymerase chain reaction (PCR) and SARS-CoV-2 infection showed significantly variable results based on the prediction made in the current study. These discrepancies in study results may be due to differences in the incubation times of the influenza virus (~ 1 day) and SARS-CoV-2 (approximately 5.7 days). By the time SARS-CoV-2 reaches the detection level in the body, the influenza virus may not be present due to the short incubation period.
Another prediction they made is that people who received the flu vaccine were less likely to have SARS-CoV-2 infection. This prediction is in line with the results of the previous study showing that influenza vaccination is associated with lower rates of SARS-CoV-2 infection and deaths associated with COVID-19.
Although the effect of influenza infection on SARS-CoV-2 transmission is clearly evident, the current study was conducted without controlling for a major confounding factor, age, which is known to affect influenza infection and SARS-CoV-2.
According to the scientists, this could be a potential limitation of the study. Scientists also believe that in addition to the influenza virus, the effect of other respiratory viruses must also be tested for more comprehensive monitoring.
With regard to control measures, the scientists believe that the effect they observed may be specific to Europe, where the number and intensity of control measures gradually increased during the epidemic.
*Important note
medRxiv It publishes preliminary scientific reports that have not been peer-reviewed and therefore should not be considered conclusive, directing clinical practice / health-related behavior, or treated as static information.